THE CHALLENGE:
“SINGLE PERSON CARE”: Is it beneficial for patients confined to bed and the best practice for their carers?
“Single person care” allows patients who are confined to bed to be cared for and repositioned and moved by one person. This strategy initially appears to offer many solutions relating to the numbers of carers required and subsequent costs involved.
Patients who are confined to bed may present many challenges for the carers in order for them to deliver holistic, safe and effective care. They need to consider many issues including:
- The patient’s comfort
- Movement of patients
- Prevention of a one-off and/ or an accumulative tissue harm in patients
- Prevention of a one-off and/ or an accumulative micro tears, soft tissue harm and muscular skeletal injury to the carers.
Currently, there seems to have been very little reference or conversation around any new research and the practice-based evidence available regarding the accumulative effect that single-person care has on both the patients and their carers.
Geoff Marlow identifies that Practice Based Evidence is a better approach than Evidence Based Practice, and says, “In theory there’s no difference between theory and practice, but in practice there is. It’s only by taking action in the real-world that you get reliable evidence of what actually works in practice”.
Thinking about this in terms of the care of patients who are confined to bed, we need to use a practice-based-evidence approach for single-person care in order to avoid tissue harm in our patients and carers unnecessarily.
Patients/clients: the traditional practice to move patients – whether by one or more people – can create forces in their soft tissues. This is because these caring actions need a carer to use force to overcome gravity in order to move their body on a horizontal resting surface.
Harm can therefore be caused at both macro (skin) level through to nano (molecular) level. However, this effect may only become at the cellular or anatomical level (where we can see them) at a later time (approximately up to ten days). In other words, the resulting wound is just a manifestation of tissue harm and not always equal to the apparent problem causing it.
Whether tissue harm occurs depends on both the force inflicted and also the quality state of the tissue involved. However, the biggest factor is how well the body is able to adapt its behaviour, anatomy and physiology to the situation. Adaptation will depend upon how well a patient’s body’s innate protection system is working together with its protective biotensegrity structure. Therefore, these three factors: force, tissue and adaptation must be taken into account to improve the prevention of tissue harm.
The carer: We also need to be conscious of physical toll effect of care on the caregivers. This is because existing, accepted care practices expose the carer to unnecessary, accumulative micro tears, soft tissue harm and muscular skeletal injury. For example, 70% of all nurses will have at least one episode of back pain per year. With an already shrinking workforce, we need to enable those who are still in the industry – and those thinking of joining the industry – a safe and pain-free environment.
With research now demonstrating that there are 5 levels of tissue harm and the interplay within tissue when force-related tissue harm occurs leading to the occurrence of a wound, it is possible to factor in prevention of such harm into the care we give patients – learning from the observations regarding unobvious causes of forces related tissue harm and the events linking both biomechanical and biological processes at several organisational (pathological) levels together with occurring external inbed events.
Methods and practices for inbed care continue to expose the nurse/ carer’s tissues to unnecessary stresses and forces which can cause muscular skeletal injuries. This is mainly due to the present practice of working against gravity during the caring acts of supporting, moving and stabilising the patient.
THE SOLUTION:
In our blog, The missing synergy when moving patients being cared for ‘inbed’ – Part 2’, we share the eight steps to achieve a tissue-friendly care environment for both patient and carer. It uses the following new technology that also support single carers:
- Changing the bed to a multi-plane tilt bedframe
- Using a support mattress that is made of individual cells containing foam which are encased in air (hybrid mattress) with a step-up/ step-down facility
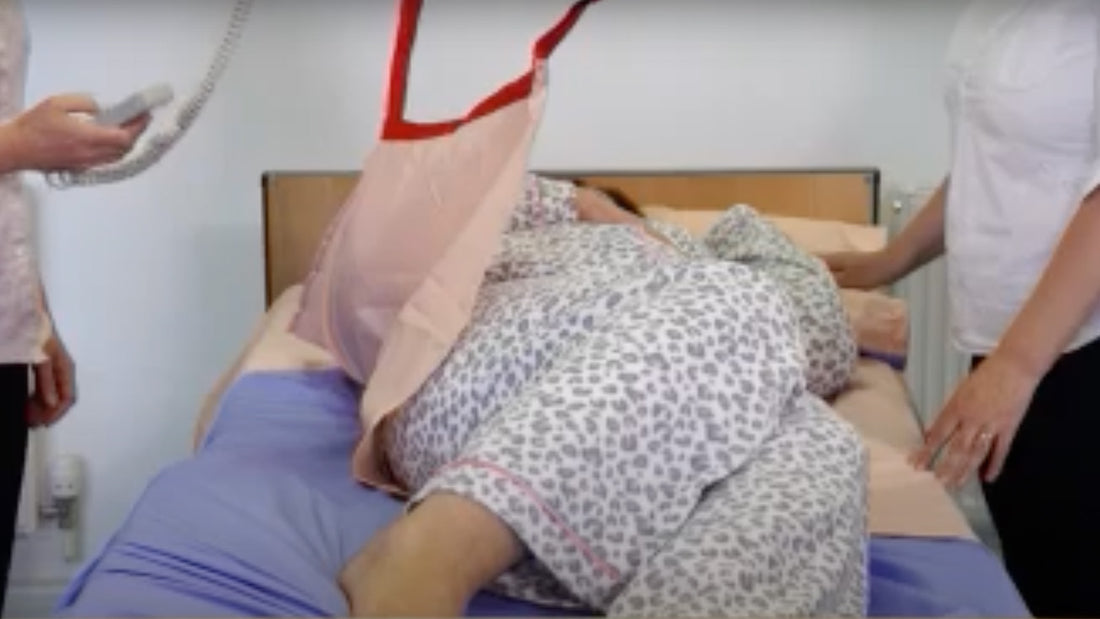
- A synergetically layered inbed care system that has bed sheets with attachments/ handles that allow it to be attached to a standard spreader bar on an overhead hoist either mobile, gantry or static (preferably static).
This practice-based-evidence approach will allow the patient to be rested, repositioned and stabilised by using gravity without the need for manual handling. This supports effective single-handed care!
This new approach will also allow:
- The care-givers the time to use the soft-skills that dramatically increase the perception of ‘good care’ and quality of care
- Care to be given that eliminates the risk of soft tissue harm to both patient and the carer whilst providing inbed care.
- Patients to be supported, repositioned and stabilised in a controlled rate and uniformed manner
- Repositioning and stabilising of the patient at a sufficiently slow rate to allow the soft tissues, homeostatic and tensegrity processes to safely dissipate potentially tissue harming forces
- To effectively eliminate the risk of biomechanical compromise and any potential soft tissue harm to the carer avoided
- The initial financial investment in the bed and inbed care systems for both hospital and community care to be outweighed by the cost savings from this approach in both terms of finance and quality of care.
CONCLUSION:
Using this practice-based-evidence approach for care of patients confined to bed, we can prevent tissue harm (in both patients confined to bed and their carers) and improve their quality of life.
As outlined above, by working with gravity to protect both patient and carer’s biotensegrity, soft tissue harm can be avoided.
However, it is important to recognise that changing practices is hard. That’s because it's new and differs from what's been accepted, so it's going to run into controversy?
It is a positive step that companies such as Sunday Care Therapy are already recognising the need for tissue-friendly single-person approach as demonstrated in their presentation at Naidex 2022.
If you would like to discuss how to transition your care provision and/ or single-person care training to reflect this practice-based-evidence approach, please do contact me.

References:
https://geoffmarlow.substack.com/p/practice-based-evidence?s=w
https://www.linkedin.com/posts/harmjaap_elucidating-the-causes-of-neurodegeneration-activity-6949677486645374977-CTxn?utm_source=share&utm_medium=member_desktop
https://www.hje.org.uk/back-care-awareness-week-2020-back-pain-in-nurses/
https://www.linkedin.com/pulse/harm-scale-harm-jaap-smit/
https://www.cureus.com/articles/29258-structural-elements-of-the-biomechanical-system-of-soft-tissue
https://centrobed.com/p/arctic-turning-bed
https://www.directhealthcaregroup.com/products/dyna-form-mercury-advance/
https://www.linkedin.com/posts/alexnesbitt_hackingluck-leadership-strategy-activity-6959950406525366272-PmlM??
https://www.linkedin.com/company/sunday-care-therapy/?originalSubdomain=uk
https://www.azquotes.com/quote/851832